If your mood feels “mental” but your body feels off too
Some days your thoughts look like the problem, but your body keeps interrupting: you wake up wired, your chest feels tight, your stomach is unpredictable, or you’re tired in a way coffee can’t touch. It’s easy to file that under “stress” and try to think your way out of it. But mood and body signals push on each other all day—sleep changes how reactive you feel, food timing can mimic anxiety, and pain can shrink your patience.
Online advice treats these as separate buckets, so you either overhaul everything or do nothing. Notice the loop you’re in, then change one piece you can measure without guesswork. That starts with mapping what your body and mood actually do together in real life.
Start by mapping what your body and mood do to each other in real life
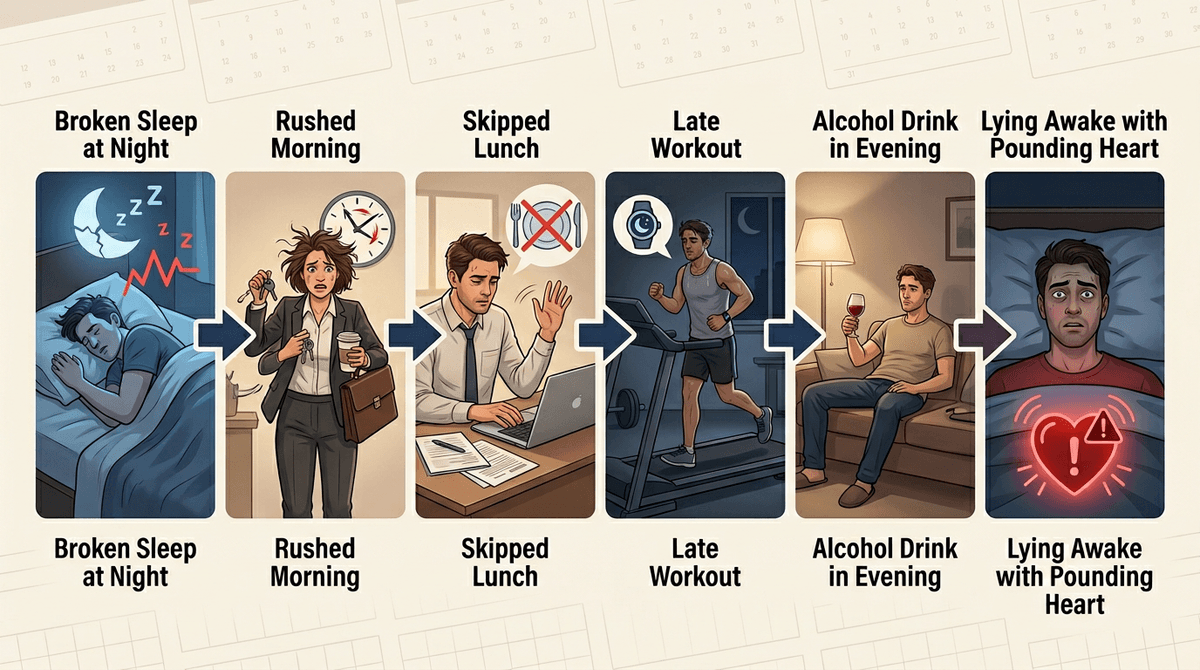
That mapping looks like what you already do on a normal week: a rough night, a rushed morning, a skipped lunch, a late workout, a drink to “take the edge off,” then lying awake with your heart thumping. The goal isn’t to label yourself. It’s to catch the order things happen, because the same symptom can come from different chains.
For seven days, jot down three quick notes: when you slept (and how broken it felt), when you ate (especially long gaps, high-sugar snacks, caffeine), and when your body felt “on” (tight chest, shaky hands, stomach flipping, headaches, aches). Then add a simple mood score (0–10) and one sentence about what was happening right before it spiked or crashed.
This takes time and it can feel annoying, especially on busy days. But it turns “I’m anxious all the time” into “I’m okay until 11 a.m., then I crash after coffee and no food,” which makes the next decision—sleep, movement, food, or a check-up—much clearer.
When sleep is the first domino (and when it isn’t)
Once you can see “I’m okay until 11 a.m.” patterns, sleep often shows up as the quiet driver. A short night doesn’t just make you tired. It can make your body run hotter the next day—faster heartbeat, more muscle tension, more snapping at small stuff—so normal stress feels like a threat. If your mood is noticeably steadier after even two or three nights of more consistent sleep and wake times, that’s a strong hint sleep is the first domino.
But sleep isn’t always the root. If you’re in bed long enough and still wake up unrefreshed, or you fall asleep fine but wake up sweaty, gasping, in pain, or to use the bathroom repeatedly, the sleep problem may be downstream. The same goes if your sleep only falls apart after caffeine, late intense workouts, or long gaps without food.
Exercise helps—unless it’s draining you: how to choose the right dose

That “late intense workout” note is a common fork in the road: some people sleep better and feel calmer, and others end up buzzing, sore, and more fragile the next day. Exercise can blunt stress in the moment and improve sleep over time, but only if it lands like recovery, not another demand on a body that’s already running hot.
If you feel more settled within a few hours—looser shoulders, steadier stomach, easier wind-down—that’s a good dose. If you get a wired second wind, more rumination, a racing heart at bedtime, or you’re wiped out for the next 24–48 hours, pull the dial back. Start with “easy” movement you can repeat: a brisk 20–30 minute walk, light cycling, or lifting that leaves 2–3 reps in the tank. Keep harder sessions earlier in the day, and cap them to a few times a week.
The right dose often means shorter, more consistent sessions, not heroic ones. Once movement is steady, it gets easier to see what food and substances are doing to your mood swings.
Food, blood sugar, and substances: what’s worth changing first without going extreme
Once movement settles into a routine, eating patterns often become easier to spot. Energy may feel stable for a while, then drop suddenly—showing up as shakiness, irritability, or mental fog. This often follows long gaps between meals, a sugary snack, or another coffee on an empty stomach. It can resemble anxiety, but is frequently a sign that the body needs more consistent fuel. A simple starting point helps: eat a balanced meal with protein and fiber within a couple of hours of waking, and avoid going more than four to five hours without eating. If energy tends to dip in the afternoon, adding a planned snack—such as nuts, yogurt, or a sandwich—can smooth the transition.
Caffeine and irregular eating habits can amplify these ups and downs, even when they seem helpful at first. A short trial period can make patterns clearer: limit caffeine to earlier in the day and notice whether symptoms like chest tightness, stomach discomfort, or restlessness at night begin to ease. Skipping meals or relying on quick snacks may also lead to a cycle of short-lived energy followed by sharper dips later on. Adjusting these habits can feel inconvenient at first, and it may take a few days for the body to adapt to a steadier rhythm.
If notes show clear links between mood changes and eating patterns, drinks, or other daily habits, that can be useful information to bring into a routine check-up.
The “maybe it’s medical” moment: symptoms that should trigger a check-up
If your notes keep pointing to the same physical spikes—racing heart, shaky hands, stomach flips—but the usual levers (sleep, steady meals, dialing back caffeine, lighter workouts) don’t change the pattern, that’s often the “maybe it’s medical” moment. Not because it’s “all in your body,” but because a few common health issues can copy anxiety or keep your mood stuck.
Book a primary care visit soon if you have a big shift you can’t explain (new panic-like episodes, mood drop, or fatigue that lasts weeks), symptoms that wake you at night (gasping/snoring, sweating, chest discomfort), or body changes that don’t match your habits (unintended weight change, heat or cold intolerance, hair/skin changes). The same goes for frequent palpitations, shortness of breath with light effort, persistent gut issues, new headaches, or pain that narrows your day. And if a medication or supplement change happened around the time things worsened, that timing matters.
Tests don’t always give a clean answer on the first try, and that can feel discouraging. Still, catching sleep apnea, thyroid issues, anemia, nutrient deficits, hormone shifts, or medication side effects can turn “try harder” into a real plan for what to do next.
How to show up to an appointment—and leave with a plan you can actually follow
That “real plan” usually depends less on the test order and more on what you walk in holding. If you show up with “I’m anxious and tired,” you may leave with broad advice. If you show up with a one-page pattern, you make it easier to aim the visit.
Bring your seven-day notes and circle two or three repeatable chains, like “coffee + no breakfast → shaky by 11” or “hard workout after 6 p.m. → wired at bedtime.” List any meds, supplements, and weed with rough amounts and timing. Then write three questions you want answered: “What medical causes should we rule out?” “Which labs (if any) fit my symptoms?” “What should I try first for four weeks, and how will we measure if it worked?”
You may get 10–15 minutes. Ask for the next step in writing—what to change, when to follow up, and what new symptoms mean “call sooner.”
A simple way to move forward: one body lever, one mind lever, one medical check (if needed)
When the visit ends, it’s tempting to either overhaul your whole life or wait for a perfect answer. A cleaner way forward is a small three-part plan you can actually stick to for two to four weeks: one body lever, one mind lever, and one medical check if your notes point that way.
Pick a body lever you can measure daily: a fixed wake time, a real breakfast with protein, or a 25-minute easy walk. Pick a mind lever that changes the moment your symptoms spike: a two-minute slow-breath reset, a “name it and do one next step” script, or 10 minutes of worry time scheduled earlier. Keep it simple enough that a rough day can’t break it.
If red-flag symptoms showed up, or the pattern doesn’t budge after the trial, book the check-up and bring the notes. The cost is patience: improvement usually looks like fewer bad hours, not a sudden flip.











