The pain pattern that raises suspicion
It can start with a small clue that’s hard to dismiss: your hands feel thick and slow first thing in the morning, like the joints need time to “wake up.” The stiffness may last longer than you expect, and it can be oddly better after you’ve been moving for a while, even though you didn’t do anything to “work it out.” That inconsistency—worse after rest, easier with gentle use—often makes people question whether it’s just overuse or sleep position.
Another detail that can raise suspicion is the symmetry. Swelling or tenderness may show up in similar spots on both sides, especially in the wrists and the small knuckles, and rings may suddenly feel tight. This pattern can happen because inflammation is building inside the joint lining, where immune signals pull in fluid and inflammatory cells. That internal swelling can create pressure and stiffness that feels deeper than muscle soreness, and it can fluctuate—flaring for days, then easing enough to make you second-guess what you felt.
Why inflammation targets joints, not just muscles
Sometimes the ache feels like it should be coming from the muscles around the joint—forearm, palm, the “meaty” part near the thumb—but the tenderness doesn’t behave like a strain. You can rest it, skip lifting, even sleep differently, and still wake up with that same stiff, pressurized feeling that makes your hands seem clumsy for longer than seems reasonable.
In inflammatory arthritis, the main trouble spot is often the synovium, the thin lining that coats the inside of a joint capsule. When immune signaling gets repeatedly turned on there, the synovium can hold onto fluid and attract inflammatory cells, which makes the space inside the joint feel tight. That pressure limits smooth motion and can create pain with simple movements—less like “worked-out” muscle soreness and more like something deep that catches when you try to bend or grip.
Because the synovium is present in many joints—and not evenly stressed day to day—the discomfort can move around or show up in matching joints on both sides. That inconsistency can be confusing, especially when one day feels almost normal and the next day your rings won’t slide on.
What drives this pattern beneath the surface
On some mornings, the swelling isn’t dramatic—just enough that a fist feels incomplete, like the joints are moving through thick air. Then later, after dishes or a commute, your hands may loosen up in a way that doesn’t match how “injuries” usually behave. That back-and-forth can be unsettling, especially if you’re trying to decide whether you should push through the day or protect the joints.
Beneath that experience, rheumatoid arthritis is often driven by immune signals that stay active in the synovium longer than they should. The synovial tissue can become more crowded with inflammatory cells and extra fluid, which raises pressure inside the joint capsule. After you’ve been still, that pressure and inflammation can translate into stiffness; gentle movement may temporarily improve how fluid shifts and how the joint surfaces glide, even though the underlying process hasn’t truly switched off.
Flares can also feel “out of proportion” to what you did because the immune system doesn’t always follow a predictable schedule. Stress, intercurrent illness, sleep disruption, or even no clear trigger can tilt the balance toward more signaling for a time, then ease again—creating a stop-start pattern that’s easy to misread as random overuse or aging.
Symptoms beyond joints that surprise people

It can be a strange moment when the joints aren’t the loudest symptom—when you’ve slept a full night but still feel wrung out, or when a low-grade, “coming-down-with-something” feeling hangs around without turning into a clear illness. That fatigue can be inconsistent, showing up on days when the hands don’t look especially swollen, which makes it easy to dismiss as stress or a busy week.
In rheumatoid arthritis, the same immune signals that irritate the synovium can circulate more broadly, and that body-wide inflammation may shift how your energy and temperature regulation feel. Some people notice a reduced appetite, a vague sense of being unwell, or mild fevers, not because the joints are “spreading,” but because inflammatory messaging affects more than one system at a time.
Other surprises can be harder to connect: dry, gritty eyes or a dry mouth; tender, swollen lymph nodes; or a subtle heaviness in the chest with deep breaths. These don’t confirm anything on their own, but if they persist or pile up alongside the joint pattern, they’re worth mentioning clearly at an appointment.
Diagnosis: combining stories, labs, and imaging clues
You might notice how the conversation changes once someone starts asking for specifics you’ve never tracked—how long the morning stiffness lasts, which knuckles swell, whether it’s the same joints on both sides, and what a flare actually looks like across a week. That timeline matters because inflammatory patterns can be inconsistent, and single “good days” can make it tempting to downplay what’s been happening.
Blood tests can add clues, but they rarely act like a simple yes-or-no. Some people have antibodies often associated with rheumatoid arthritis (like rheumatoid factor or anti-CCP), while others don’t, even when symptoms fit. Markers of inflammation (like ESR or CRP) may be elevated during a flare and closer to normal when things quiet down, which can feel confusing if your joints still hurt.
Imaging is sometimes used to catch what hands can’t show from the outside. Ultrasound or MRI may pick up synovial thickening or active inflammation before X-rays show clearer changes, which is why clinicians often put the story, exam, labs, and imaging together instead of leaning on any single piece.
Treatments that change disease trajectory over time
There’s a particular kind of frustration when the swelling is down but the plan still gets “bigger.” It can feel like overkill to talk about long-term medication when you’re mostly trying to get through mornings and keep your hands working. And because symptoms can calm on their own, it’s easy to wonder whether time alone would have done the same thing.
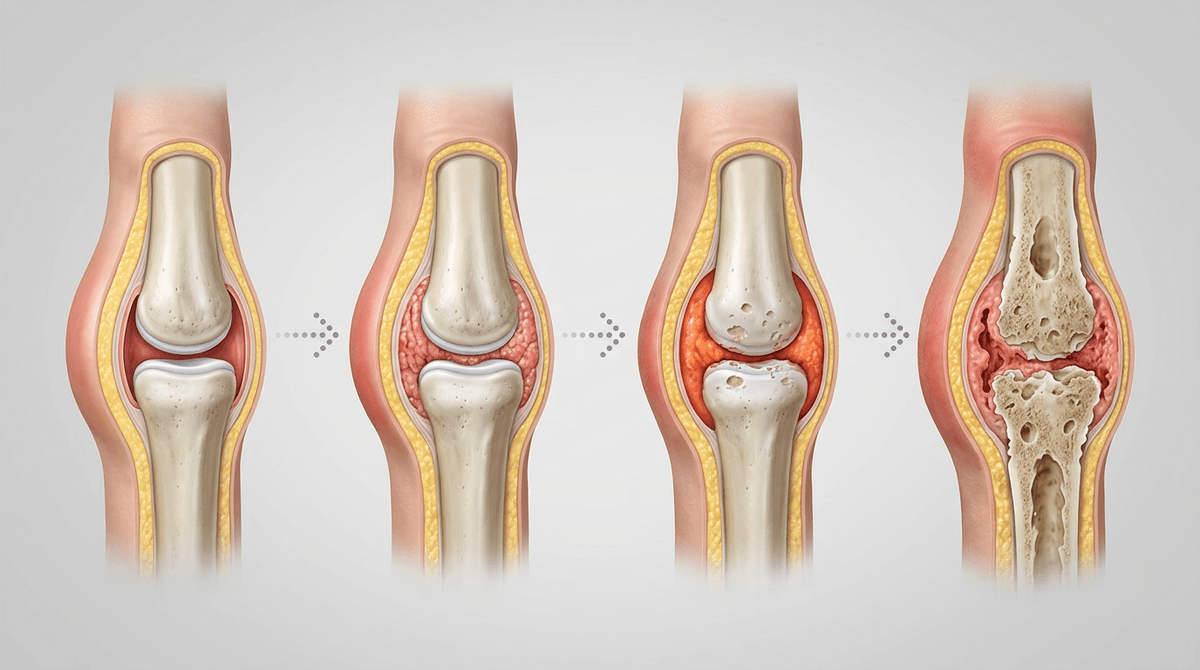
The reason treatment is often framed around the long game is that the discomfort you feel isn’t the whole story. In rheumatoid arthritis, immune signaling can keep the synovium metabolically active even when a joint looks only mildly puffy. Over time, that ongoing activity can thicken the lining and promote enzymes and cells that erode cartilage and bone. So some medications are chosen less for immediate relief and more for turning down that immune cascade before it leaves more permanent limits.
Anti-inflammatory medicines and short steroid courses may quiet symptoms quickly, but they don’t reliably prevent the underlying joint damage on their own. Disease-modifying treatments (often started early and adjusted over months) are aimed at changing the trajectory—sometimes with a noticeable lag—so the day-to-day feedback can feel inconsistent at first, even when the long-term goal is clearer function and fewer flares.
When reasonable choices create unexpected confusion
It’s often a small, practical decision that starts the confusion: you take an anti-inflammatory, the swelling looks calmer by lunchtime, and the day feels “proof” that the problem is mostly pain control. Then the next morning the stiffness is back, and it can feel like nothing counts—either the medicine “failed” or the whole situation was exaggerated.
Part of the mismatch is timing. Symptom-relief medicines can reduce pain signaling and fluid-related pressure fairly quickly, while the synovium can stay biologically active underneath. That means a joint can feel better before the immune-driven process has truly quieted, or it can still feel sore even as inflammation markers drift down. Add in work days, stress, or a minor virus, and the pattern can look inconsistent even when the underlying mechanism is still the same.
Skipping movement to “protect” the hands may lead to more stiffness after rest, which can be misread as progression. On the other side, a better week can make follow-up labs or medication changes feel unnecessary. If the back-and-forth keeps happening, it’s usually worth naming it directly at the next visit rather than trying to interpret each day as the final answer.











